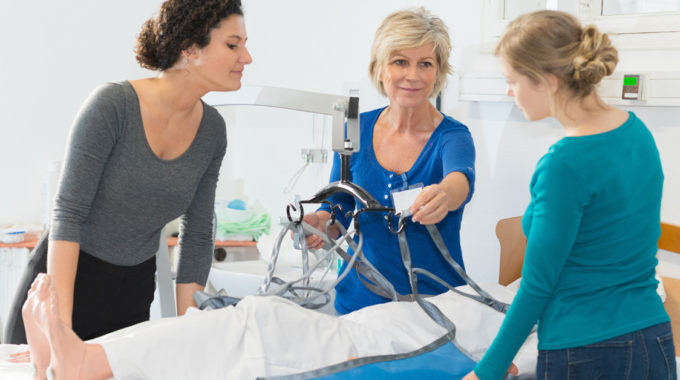
Family Caregivers Need More Training
In commentary by Karina Berg MD and others recently published in the Journal of the American Medical Association, they cite that only 7.3% of family caregivers in a large, recent study report receiving training for the caregiving tasks.1 Training is probably more common than that, but Berg’s larger point is that caregivers need and deserve training, not just once, but ongoing.
What is a Family Caregiver?
In the U.S., nearly 18 million people provide assistance for a senior or elderly relative, much of which is unpaid work.2 These are family caregivers. They are 2/3 female and average 60 years in age.7 In some cases, the support provided revolves around homemaker and errand tasks such as getting groceries, mowing the lawn, and assisting with home cleaning – things we all learned to do while growing up. However, the need for this assistance commonly rises from progressive chronic diseases. Therefore, the caregiving requirements progress in their technical nature and in their personal burden. Before long, family caregivers are managing therapeutic diets needed to control chronic diseases, assisting with ambulation and transfers up and down from furniture, performing colostomy and ostomy care, delivering routine injections, managing multiple medications, managing catheters, and even performing wound care.3 The list goes on and on.
Why Train Family Caregivers?
- Family and informal caregivers often report feeling poorly supported and poorly trained in their caregiving role.4
- Caregiver education is associated with better health outcomes and reduced hospitalizations.5
- Unmet home care needs have been associated with a 37% increase in mortality rates for the care recipient and a 77% increase in institutionalization.
- When elderly family caregivers feel stressed and unsupported, their 4-year mortality risk can increase 63% or more.6
How Many Family Caregivers Receive Training?
Dr. Berg was referencing the research of Julia Burgdoff. Burgdoff et al. investigated 1,861 family caregivers. When asked if they had received training in the last year, roughly 93% answered no. That does not mean they received no training, just none in the past 12 months.
The extent to which family caregivers require annual training is not established. As Dr. Berg commented, the technicality and burden of family caregiving can progress “insidiously.” At the professional level, this sort of care tends to be provided by certified nursing assistants, home health aides, and similar professionals who have usually completed a six-week training course. Most federal programs require that these professionals receive 12 hours of continuing education annually.
Burgdoff found that the likelihood of caregiver training doubled if the care recipient had recently been discharged from a hospital. CARE legislation (Caregiver Advise, Record, Enable) in most states require hospitals to provide caregiver support at discharge.
Burgdoff also found that paid family caregivers were more likely to receive training. Medicaid funds programs that pay non-spouse family caregivers from different households to care for their own family member or friend when doing so may prevent nursing home expenses. Medicaid is a partnership between states and the federal program. Resultantly, this particular program varies extensively from state to state, and may not exist at all in some states. New York’s CDPAP (Consumer Directed Personal Assistance Program) is one of the more popular iterations of paid family caregiving.
Where to Get Caregiver Training
The answer to this question likely highlights the problem. There is no established source for this training. Programs that do exist tend to not give the hours or weeks of training that a home health aide would receive.
One good source is Medicare-certified home health. If there has been a recent health occurrence, Medicare will typically pay 100% for several nurse visits to reinforce caregiver training. Of course, for Medicare to pay, there must be a recent change in condition such as an accidental fall or out of control lab values. Absent that, there is little in the way of a universal answer. When Medicare reimbursement is not an option, families should seriously consider paying privately for home nursing and aide services for caregiver training and care planning plus assistance with the caregiving duties.
References:
- Berg KM, Fortinsky RH, Robison J. Family caregivers needed—No training provided. JAMA Internal Medicine. 2019 Jun 1; 179 (6): 835-6.
- Wolff JL, Spillman BC, Freedman VA, Kasper JD. A national profile of family and unpaid caregivers who assist older adults with health care activities. JAMA Internal Medicine. 2016 Mar 1; 176 (3): 372-9.
- Reinhard SC, Feinberg LF. The escalating complexity of family caregiving: meeting the challenge. In Family caregiving in the new normal 2015 Jan 1 (pp. 291-303). Academic Press.
- National Academies of Sciences, Engineering, and Medicine. Families caring for an aging America. National Academies Press; 2016 Dec 8.
- Nuckols TK, Keeler E, Morton S, Anderson L, Doyle BJ, Pevnick J, Booth M, Shanman R, Arifkhanova A, Shekelle P. Economic evaluation of quality improvement interventions designed to prevent hospital readmission: a systematic review and meta-analysis. JAMA Internal Medicine. 2017 Jul 1; 177 (7): 975-85.
- Schulz R, Beach SR. Caregiving as a risk factor for mortality: the Caregiver Health Effects Study. JAMA. 1999 Dec 15; 282 (23): 2215-9.
- Burgdorf J, Roth DL, Riffin C, Wolff JL. Factors associated with receipt of training among caregivers of older adults. JAMA Internal Medicine. 2019 Jun 1; 179 (6): 833-5.






